5 Best Exercises for Baker’s Cyst Relief
By Essex Osteo – Stanford-le-Hope
A Baker’s cyst (also known as a popliteal cyst) is a fluid-filled swelling that develops at the back of the knee. It is often linked to underlying knee conditions such as arthritis, meniscus injuries, or chronic inflammation. While a Baker’s cyst can feel tight, swollen, or uncomfortable, the right exercises can significantly reduce pain, improve mobility, and support long-term recovery.
At Essex Osteo in Stanford-le-Hope, we regularly help patients manage Baker’s cysts using a combination of osteopathic treatment, rehabilitation exercises, and lifestyle advice. Below are the five best exercises for Baker’s cyst relief, commonly recommended by our osteopaths.
1. Gentle Hamstring Stretch

Tight hamstrings can increase pressure around the knee joint, worsening Baker’s cyst symptoms.
How to do it:
-
Lie on your back with one leg bent
-
Raise the other leg and gently pull it towards you
-
Keep the knee slightly bent
-
Hold for 20–30 seconds
-
Repeat 3 times on each side
Why it helps:
Improves flexibility at the back of the thigh and reduces tension behind the knee.
2. Calf Stretch

Calf tightness can restrict knee movement and contribute to swelling.
How to do it:
-
Stand facing a wall
-
Step one foot back, keeping the heel on the floor
-
Bend the front knee and lean forward
-
Hold for 30 seconds
-
Repeat 2–3 times per leg
Why it helps:
Encourages better circulation and reduces stiffness around the knee joint.
3. Straight Leg Raises

This exercise strengthens the quadriceps without putting excessive strain on the knee.
How to do it:
-
Lie on your back with one leg bent
-
Keep the other leg straight and lift it to knee height
-
Hold for 5 seconds, then lower slowly
-
Perform 10–15 repetitions
Why it helps:
Improves knee stability and reduces joint stress that can aggravate a Baker’s cyst.
4. Heel Slides

Heel slides gently restore knee mobility and help reduce joint stiffness.
How to do it:
-
Lie on your back with legs straight
-
Slowly slide one heel towards your buttocks
-
Pause briefly, then slide it back down
-
Repeat 10–15 times per leg
Why it helps:
Maintains healthy knee movement and prevents fluid build-up behind the knee.
5. Glute Bridges
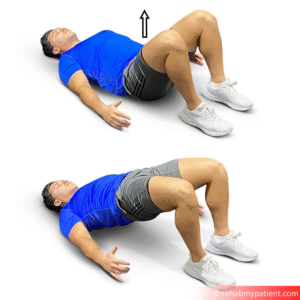
Weak glute muscles can overload the knee joint, contributing to inflammation.
How to do it:
-
Lie on your back with knees bent
-
Tighten your core and lift your hips
-
Hold for 5 seconds before lowering
-
Perform 10–15 repetitions
Why it helps:
Supports proper lower-limb alignment and reduces pressure on the knee.
When to Avoid Exercise
If your Baker’s cyst is very painful, rapidly swelling, or restricting movement, avoid exercise and seek professional assessment. Exercises should never increase pain at the back of the knee.
At Essex Osteo in Stanford-le-Hope, our osteopaths assess why the cyst developed in the first place — not just the symptoms — ensuring safe and effective treatment.
Osteopathic Treatment for Baker’s Cyst in Stanford-le-Hope
Exercise works best when combined with hands-on osteopathic treatment. At Essex Osteo, we may also use:
-
Manual therapy to reduce joint strain
-
Soft tissue techniques to improve circulation
-
Postural and movement advice
-
Tailored rehabilitation programmes
If you’re experiencing knee pain, swelling behind the knee, or stiffness, early treatment can help prevent recurrence.
Book an Appointment at Essex Osteo
If you’re looking for Baker’s cyst treatment in Stanford-le-Hope, Essex Osteo is here to help. Our experienced osteopaths provide personalised care to relieve pain, restore movement, and support long-term knee health.
📍 Essex Osteo – Stanford-le-Hope
📞 Contact us today to book your consultation.
Frequently Asked Questions About Baker’s Cyst
What is a Baker’s cyst?
A Baker’s cyst, also called a popliteal cyst, is a fluid-filled swelling behind the knee. It usually develops when excess joint fluid is pushed to the back of the knee due to conditions such as osteoarthritis, meniscus tears, or ongoing knee inflammation.
Can exercise help a Baker’s cyst?
Yes — gentle, targeted exercises can help reduce stiffness, improve circulation, and relieve pressure in the knee joint. Exercises that strengthen the surrounding muscles and improve flexibility often help reduce symptoms and prevent recurrence. However, exercises should never cause pain or increase swelling.
What exercises should I avoid with a Baker’s cyst?
Avoid:
-
Deep squats
-
Lunges that cause pain
-
High-impact activities such as running or jumping
-
Sudden twisting movements
These can increase knee pressure and worsen the cyst. An osteopath can advise which movements are safe for your specific condition.
Will a Baker’s cyst go away on its own?
In some cases, a Baker’s cyst may reduce in size or disappear once the underlying knee problem is treated. However, without addressing the root cause, cysts can return. Professional treatment helps manage symptoms and reduce the likelihood of recurrence.
Can osteopathic treatment help a Baker’s cyst?
Yes. Osteopathic treatment can:
-
Reduce knee joint stress
-
Improve movement and circulation
-
Address muscle imbalances
-
Support healing of underlying conditions
At Essex Osteo, treatment plans are tailored to the individual and often combined with rehabilitation exercises for best results.
When should I see an osteopath for a Baker’s cyst?
You should seek professional advice if:
-
Swelling persists or worsens
-
Knee pain limits daily activities
-
The knee feels tight or unstable
-
Symptoms return repeatedly
Early assessment can prevent long-term discomfort and complications.
FAQs
Is a Baker’s cyst serious?
A Baker’s cyst is usually not dangerous, but it can be uncomfortable and restrictive. Rarely, a ruptured cyst can cause calf pain and swelling that mimics a blood clot, so persistent or sudden symptoms should always be assessed by a healthcare professional.
Can Baker’s cysts come back after treatment?
They can, especially if the underlying cause isn’t addressed. That’s why combining manual treatment, exercise, and movement advice is key to long-term relief.